
In skin biology, senescence is a process by which a cell ages and permanently stops dividing but does not die. This is why they are also referred to as "zombie cells". Age-related accumulation of senescent cells is caused by of increased levels of senescence-inducing stressors and/or reduced elimination of senescent cells. Under normal physiological conditions, senescent cells play an important role maintaining cellular homeostasis and inhibiting proliferation of abnormal cells. However, over time, large numbers of zombie cells can build up in the skin and contribute to the overall reduction in skin's regenerative properties, impacting both its beauty and health.
There are 2 forms of cell senescence: Acute senescence: Senescent cells are produced in response to acute stressors to facilitate for example tissue repair, wound healing. They are cleared by our immune system. Chronic senescence: A not programmed process as response to prolonged stress or damage and these senescent cells are not cleared by our immune system, leading to the accumulation of zombie cells impacting our skin health and beauty. It has been suggested that inflammageing is mainly related to senescent cells and their associated SASP (Senescence-Associated Secretory Phenotype) which increase in the body with age and contribute to inflammageing. Senescent cells cause inflammageing and inflammageing causes cell senescence. [1] Senescence can be triggered by a number of stress signals to the cell [1]:
Mechanisms of skin cell senescence:
The presence of senescent cells accelerates the ageing process due to their communication with nearby cells through various molecules: [18]
Fibroblast senescence could be the main driver of the skin ageing. [3] The increased number of senescent fibroblasts results in the production of SASPs rich in pro-inflammatory cytokines, including interleukin (IL)-1, IL-6, IL-8, IL-18, matrix metalloproteinases (MMPs), and a variety of other inflammatory chemokines [2] resulting in the breakdown of collagen, loss of elasticity and wrinkle formation. [3] Autophagy in dermal fibroblasts is essential for maintaining skin balance and managing the ageing process, particularly in response to external stressors like UV radiation and particulate matter (PM), by repairing cellular machineries. [4] Insufficient autophagy leads to an exaggerated skin inflammation triggered by inflammasome activation, resulting in accelerated ageing characteristics. When exposed to UVB (in vitro), skin cell types like fibroblasts and keratinocytes show DNA damage and increased senescence markers, such as increased SASPs. [3] Dermal fibroblasts also release insulin-like growth factor (IGF)-1, essential for epidermal cell proliferation and differentiation. [5] IGF-1 signalling in senescent fibroblasts is significantly decreased [6]. Inhibition of the IGF-1 pathway decreases collagen production in the dermis, causing epidermal thinning. Additionally, mitochondrial dysfunction and increased levels of superoxide anions prompt fibroblast ageing, thereby speeding up the skin ageing process. [5] Fibroblasts isolated from photo-aged skin produce a greater amount of pro-melanogenic growth factors. [14] Ageing-associated pigmentation has also been reported to be driven by (UVA-induced) fibroblast senescence. [15-16] Keratinocyte senescence The epidermis shows less impact of senescent keratinocytes due to their quicker turnover in comparison to fibroblasts. Senescent keratinocytes experience reduced ECM production and cell adhesions [8], along with elevated MMP expression in UV-induced senescence [9], and increased SASP levels, including pro-inflammatory cytokines. [10] Airborn particulate matter (PM2.5) can penetrate a disrupted skin barrier. PM2.5-induced ROS leads to epigenetic modification: reduced DNA methyltransferase, elevated DNA demethylase expression, p16INK4a promotor hypomethylation and therewith accelerated keratinocyte senescence. [11] Keratinocytes are the main type of cells that signal the need for melanogenesis. [12] UVR-induced DNA damage in keratinocytes activates melanogenesis. [13] Melanocyte senescence Senescent melanocytes express markers of inflammageing and dysfunctional telomeres. Senescent melanocyte SASPs induce telomere dysfunction and limit the proliferation of the surrounding cells, hence, senescent melanocytes affect and impair basal keratinocyte proliferation and contribute to epidermal atrophy. [17] STRATEGIES TO COMBAT CELL SENESCENCE PREVENTION Sunscreen: Protection against UV radiation combined with blue light defense (Licochalcone A: powerful anti-oxidant, Nrf2-Activator & increasing Glutathione + Colour pigments) and prevention + repair DNA damage (Glycyrrhetinic Acid) INTERVENTION Senotherapeutics can be classified into three development strategies: [25]
Skin care ingredients: [18]
Of course a healthy life-style and diet (consider also intermittent fasting) will support both your body & skin longevity and beauty Prevention and intervention of skin cell senescence offers a promising approach to improve skin health and beauty. Always consult a qualified healthcare professional or dermatologist to determine the most suitable approach for your particular skin condition and rejuvenation goals. Take care! Anne-Marie References
Comments

Many of the skin regenerating or rejuvenating treatments, like energy based devices in the doctors-office are based on the principle to cause controlled damage and therewith provocation of a skin rejuvenating repair response. One of the fascinating mechanisms behind laser "damage" is the heat shock response leading to increased production of regenerating heat shock proteins (HSPs). Heat shock proteins respond to heat stress, are crucial cellular defense mechanisms against stress (environmental and physiological), act as chaperones, aiding in protein folding, prevention of protein damage, cellular protection and repair. [1]
HEAT SHOCK PROTEINS AND OX-INFLAMMAGEING UV radiation and blue light cause oxidative stress and inflammation, and can overwhelm skin's own capacity to counteract the increased formation of reactive oxygen species (ROS) and inflammatory mediators. Chronic oxidative stress state and chronic low grade of inflammation are hallmarks of skin ageing and their combination can be called ox-inflammageing. Oxidative stress and inflammation alter cellular signal transduction pathways and thereby the expression of the ECM genes as well as the structure of the ECM proteins like collagen, fibronectin and elastin. Their reduced expression and increased degradation manifests eventually at the skin surface as wrinkles, loss of firmness, and elasticity. Heat shock proteins are chaperone proteins that facilitate the formation of the ECM and prevention of molecular oxidative damage or degradation and are classified based on their molecular weights.
STIMULATION OF REJUVENATING HEAT SHOCK PROTEINS Heat shock protein synthesis can be initiated not only by heat but also by many chemical and physical stimuli, such as heavy metals, amino acid analogues, oxidative stress, viral infection and UV and ionizing irradiation. [10] Laser Laser treatments have been shown to induce a heat shock response in the skin from epithelial cells to deeper connective tissues, leading to the production of heat shock proteins. This response is characterized by the temporary changes in cellular metabolism, release of growth factors, and increased cell proliferation and thus contribute to tissue regeneration and rejuvenation. [11] CBD It has been proven that a large number of genes belonging to the heat shock protein super-family were up-regulated following cannabidiol (CBD) treatment. [12] UV radiation Ultraviolet radiation (UV)‐induced cell death and sunburn cell formation can be inhibited by previous heat shock exposure and UV itself can induce HSP expression. However, levels of HSP-27 have been found to be elevated in sun‐protected aged skin indicating a link between HSP-27 expression and age‐dependent epidermal alterations. [13] I would recommend daily protection from UV radiation and blue light (or high energy visible light). Ultrasound Ultrasound exposure at different frequencies, intensities, and exposure times can induce HSP-72 expression. Higher ultrasound frequencies, such as 10 MHz, have been found to significantly increase HSP-72 levels. Additionally, increasing the temperature during ultrasound exposure has shown to enhance HSP-72 expression. Interestingly, ultrasound at 1 MHz was unable to induce HSP-72 significantly, while 10 MHz ultrasound induced HSP-72 after 5 minutes of exposure. [10] Radiofrequency Radiofrequency has been shown to increase HSP-70 and decrease melanin synthesis and tyrosinase activity. [14] RF-US treatment significantly increased levels of HSP47 proteins. [15] Red & near infra red light Although I've not seen much peer reviewed published evidence, red light and near infra red light therapy may release the HSPs in the skin if tissue reaches >42 - 45 degrees (even for 8 - 10 seconds). Nicotinamide Nicotinamide and its derivatives have been found to stimulate the expression of heat shock proteins, including HSP-27, HSP-47, HSP-70, and HSP-90 in the skin. These proteins play as mentioned before an essential role in collagen production, skin protection, skin health and rejuvenation. [6] NAD as nutrient interestingly has proven to tweak the epigenome by modulating DNMT1 enzymatic DNA methylation and cell differentiation. [16] In topical applications an ingredient called Dihydromyricetin also called Epicelline® has been successful in inhibiting DNMT1 enzyme activity biochemical assays. [17] Stimulation of heat shock proteins offers a promising and novel invasive, non invasive and topical approach for skin regeneration, rejuvenation and reduction of ox-inflammageing. Always consult a qualified healthcare professional or dermatologist to determine the most suitable approach for your particular skin condition and rejuvenation goals. Take care! Anne-Marie References

One of the people I follow ever since I started to work on skin epigenetics back in 2017 and longevity is Harvard professor David Sinclair. He is best known for his work on understanding why we age and how to slow its effects. He was talking about hormesis, a phenomenon where exposure to low doses of stressors induces beneficial effects. A hormetic (cellular defense) response can modulate ageing processes by activating genes related to maintenance and repair pathways through mild stress exposure in our body and skin, leading to enhanced longevity (thus anti-ageing) and health. [1 - 2]
Originating from the early 2000s, the concept of hormesis has evolved to evidenced based dermatological applications. [3] Various factors, including environmental stressors, lifestyle choices, and genetic predispositions, can influence the hormetic responses in skin cells. Understanding these influences is essential for optimizing skin health and beauty through hormetic pathways. Many terms are used for hormetic responses in the scientific literature, including the Arndt-Schulz Law, biphasic dose response, U-shaped dose response, preconditioning/adaptive response, overcompensation responses, rebound effect, repeat bout effect, steeling effect, among others. [4] Ageing is an emergent, epigenetic and a meta-phenomenon, not controlled by a single mechanism. Cellular damage has three primary sources: [3]
Effective homeodynamic space or buffering capacity (body's ability to maintain stability or balance in changing conditions) is characterized by:
Stress response is a reaction to physical, chemical, or biological factors (stressors) aimed at counteracting, adapting, and surviving, is a critical component of the homeodynamic space. There are seven main cellular stress response pathways:
Hormetins can be categorized into three types:
Being aware of the phenomenon of hormesis can result in discovering the usefulness of new compounds, or synergistic effects of combining hormetic treatments which otherwise may have been rejected due to their effects of stress induction. What is bad for us in excess, can be beneficial in moderation, or (quote): "What doesn't kill you makes you stronger". [6]. The future of hormesis in dermatology holds great promise for innovative interventions, advanced hormetic technologies or personalized skin care regimens. Always consult a qualified healthcare professional or dermatologist to determine the most suitable approach for your particular skin condition and rejuvenation goals. Take care! Anne-Marie Read more: The impact of senescent zombie cells on skin ageing The role of heat shock proteins in skin rejuvenation Neurocosmetics, the skin-brain connection & neuro-ageing The role of the lymphatic system in ageing skin The power of light and photo-biomodulation Bio-stimulators Skin glycation Exosomes References

If you've scrolled through Instagram, you may have caught a glimpse of dermatologists raving about LED masks emitting red light, the secret, evidenced based weapon behind skin rejuvenation known as photo biomodulation. It uses low-powered light within the red to near-infrared range (wavelengths from 632 to 1064 nm) to induce a biological reaction aka stimulate cellular processes. The wonders of red light, also known as LLLT (low-level laser therapy), PBM (red light photo-biomodulation), or PBMT (photo-biomodulating therapy), extend far beyond non-invasive skin rejuvenation. I am not a fan of devices for home use, mostly because of lacking safety and/or efficacy, PBM definitely earned it's prominent spot in my skincare routine.
A summary of the benefts of red light with and without near infrared light for skin Numerous studies have demonstrated the effectiveness of red and infrared light therapy for skin rejuvenation. A combination of red light and near IR light has proven to stimulate the production of collagen (I & III) plus elastin production (Li WH et al Int J Cosmet Sci 2021), enhance mitochondrial ATP production, cell signaling, growth factor synthesis, rebalance ROS (reactive oxidative species) and reduce inflammation. Stem cells can be activated allowing tissue repair and healing. Wrinkle and scar reduction was observed and it can reduce UV damage both as treatment and prophylactic measure. In pigmentary disorders such as vitiligo, it can increase pigmentation by melanocyte proliferation and reduce depigmentation by inhibiting autoimmunity (Pinar Avci et al. Semin Cutan Med Surg. 2013 & Mitchell J Winkie et al. Review Photodermatol Photoimmunol Photomed A focused review of visible light therapies for vitiligo 2024). It has the potential to activate both keratinocytes (epidermis) and fibroblasts (epidermal junction and dermis). With consistent use, you can expect a reduction of lines and wrinkles, improvement of skin tone and texture. PBMT (when done effective and safe) will compliment both your skin rejuvenating and regenerating at home skincare regimen and in-office procedures or even post-surgical skin recovery. ATP ATP (adenosine triphosphate) is the primary source of energy for cellular processes and plays a crucial role in various biological functions. When red light with specific wavelengths (630 nm to 638 nm and 810 nm) is absorbed by the skin cells, it stimulates the mitochondria, which are the powerhouses of the cells responsible for ATP synthesis. This increase in ATP production is providing cells with more energy to carry out their functions effectively and has several beneficial effects on the skin like boosting cellular metabolism, promoting more efficient nutrient uptake and waste removal. The increased ATP levels facilitate collagen synthesis by fibroblasts, a vital component for skin structure, elasticity and firmness and reduction of lines and wrinkles.. ATP aids in the repair and regeneration of damaged skin cells. It accelerates the healing process, making it beneficial for wound healing, post-surgical recovery, and addressing skin issues such as acne scars. ROS (Reactive Oxidative Species) By modulating ROS levels, red light therapy helps reduce oxidative stress and its detrimental effects on the skin. ROS are highly reactive molecules that are naturally produced by cells as byproducts of metabolic processes. While low levels of ROS play important roles in cellular signaling and immune responses, excessive ROS can lead to oxidative stress and damage to cells and tissues. Restoring the balance of ROS result in improved skin health, reduced inflammation, and enhanced skin rejuvenation. Red light therapy has been shown to modulate reactive oxidative species (ROS) levels in the skin by promoting antioxidant defense mechanisms and reducing oxidative stress:
The difference between LLLT and PBM LLLT refers specifically to the use of lasers, which produce coherent, focussed and an intense beam of monochromatic light, while PBM has a broader range of light sources, may include laser as well as light-emitting diodes (LEDs) and other non-laser devices. LEDs are often used in PBM because they are cost effective, versatile and have the ability to cover large treatment areas. LLT uses higher power densities with more energy and has a shorter treatment duration in comparison to PBM to achieve desired therapeutic effects. While there are similarities in terms of mode of action", there is a difference of light source, treatment application and parameters. Based on consensus, PBM and PBMT are considered the correct way to describe this photonic specialty for therapeutic applications. In this post I will focus on PBM and specifically LEDs. LED masks and LED panels LED masks specifically produced by the brand Omnilux (FDA cleared) are currently very popular for very good reasons; they are safe and effective when the LEDs emit the right wavelengths and used in the recommended frequency. Omnilux combines 2 therapeutically effective and complimentary wavelengths: 633nm and near-infrared 830 nm. Both wavelengths (more precise 630nm + 850nm) I would recommend to minimally look for in any red LED device, which will disqualify most LED masks and panels in the market! I've include some (not affiliated) links to devices below. Both masks and panels can be effective, however most panels are stronger in comparison to masks 60 mW/cm² vs mW/cm²), hence have the benefit of a shorter treatment time to get a similar result. Intensity and power of red light therapy devices are typically measured in terms of irradiance (measured in milliwatts per square centimeter, mW/cm²) and radiant flux (measured in watts, W), which quantify the amount of light energy emitted by the device. Wearing a mask during a hot summer or in a warmer climate will make you sweat and depending on the materials of the mask and straps, they may be very uncomfortable to wear. Panels have the benefit that they give a more even distribution of emitted light as masks are worn on the face and thus the LED bulbs are pushed on a small skin surface area, panels can cover a larger area (depending on their size) and are more versatile in use, as area's like neck, décolletage, or knees are easier to treat with a panel. With a mask you may be more mobile, although I would not recommend walking around while using the mask. My personal preference would be a panel for the reasons mentioned before and panels are more suitable (more hygienic) for family sharing. My son can use it after an intense workout to speed up his recovery and I like to use it for purposes beyond photo-biomodulation or skin rejuvenation, for example to improve my sleep. With a panel I get more "bang for my buck". 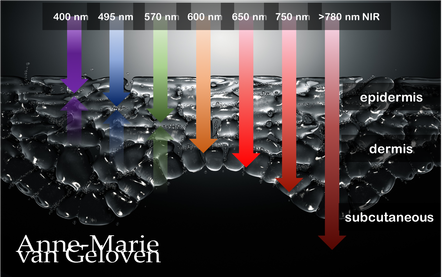
Red light and NIR (Near Infra Red light) have the ability to penetrate varying depths of the skin, resulting in distinct benefits, thus combinations of wavelengths will provide complementary effects.
630 nm Wavelength This wavelength is often used for its skin rejuvenation benefits. It has a relatively shallow penetration depth and is absorbed closer to the surface of the skin primarily affecting the epidermis. 630nm light is associated with increased circulation, reduce inflammation, improved skin tone & texture, aiding in the delivery of nutrients and oxygen to skin cells, and stimulating the production of collagen, leading to improved skin elasticity and a reduction of the appearance of fine lines & wrinkles. 660 nm Wavelength At 660nm, red light can penetrate a little deeper into the skin, reaching the dermis. It is known for its ability to stimulate collagen production, enhance cellular metabolism, and promote anti-inflammatory effects, helping to reduce redness and inflammageing. It also promotes wound healing, making it beneficial for post-surgical or post-trauma skin recovery. 810 nm Wavelength Improve healing & recovery & accelerate wound healing. 830 nm Wavelength Accelerate healing, reduce infection, improve aesthetic outcome following plastic surgery, increase endorfines (mood-enhancing), improve bone repair and growth. 850 nm Wavelength Improve general inflammation body, enhance muscle recovery, improve wound healing, reduced fine lines, wrinkles and hyperpigmentation. Always consult a qualified healthcare professional or dermatologist to determine if and what the most suitable red light therapy approach is for your particular skin condition and rejuvenation goals. Take care! References: Hamblin, Michael R. "Mechanisms and applications of the anti-inflammatory effects of photobiomodulation." AIMS biophysics 4.3 (2017): 337-361. Barolet, Daniel. Regulation of Skin Collagen Metabolism In Vitro Using a Pulsed 660 nm LED Light Source: Clinical Correlation with a Single-Blinded August 2009Journal of Investigative Dermatology 129(12):2751-9 Wunsch A, Matuschka K. (2014). A controlled trial to determine the efficacy of red and near-infrared light treatment in patient satisfaction, reduction of fine lines, wrinkles, skin roughness, and intradermal collagen density increase. Journal of Cosmetic and Laser Therapy, 16(5), 232-237. Avci P, et al. (2013). Low-level laser (light) therapy (LLLT) in skin: stimulating, healing, restoring. Seminars in Cutaneous Medicine and Surgery, 32(1), 41-52. Links to some devices which combine 630 nm and 850 nm: FDA-approved devices ensure safety and regulatory compliance, however the panels are more powerful: Omnilux(tm) Mask (FDA clearance) Very affordable panel (no FDA clearance) Affordable panel (no FDA clearance) 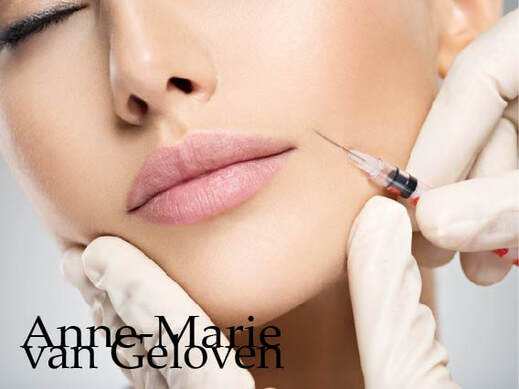
Skin ageing is a biological degenerative process, marked by loss. The number of patients seeking nonsurgical rejuvenation of the face and the body is continuing to increase due to a growing ageing population concerned with physical appearance. Women wish to maintain a youthful appearance and attractiveness represent 92% of all cosmetic procedures.(1) Men are keen to maintain physical characteristics associated with virility.(2) Millennials are also increasingly concerned with preserving their beauty and youth.(3) Among the various treatment approaches, different minimally invasive techniques have been developed and dermal fillers currently come second after botulinum toxin type A (BTA).(3) Their use is increasing worldwide.
"The fear of looking done is the number 1 reason why patients don't seek treatment"* The range of fillers available for soft-tissue augmentation is constantly expanding. The latest advances in filler technology include bio-stimulators that exert their aesthetic effect by promoting predominantly collagenesis or biological stimulation of new collagen and sometimes also elastin production. Therewith they provide a biological answer to the skin ageing degeneration process, with gradual and often very natural results. Over the course of last years the knowledge on injectable bio-stimulators has grown, and therewith their safety and popularity as they provide subtle longer lasting results. Facial fillers can be broken into 3 main groups:
Bio-stimulating fillers promote the body’s natural production of some ECM components (mostly collagen) over a period of several months. Their differences are characterized by their property of inducing natural collagen production. SYNTHETIC BIOSTIMULATORS
Calcium Hydroxylapatite Calcium hydroxylapatite: Calcium hydroxylapatite is a type of mineral that is commonly found in human teeth and bones and in injectbales the calcium hydroxylapatite particles are suspended in a gel-like solution. The effects of this material last approximately 18 months with minimal inflammatory response. Radiesse is a biodegradable filler consisting of 30% synthetic CaHA microspheres (diameter of 25-45μm) suspended in a 70% aqueous carboxymethylcellulose gel carrier. The soluble carrier gel evenly distributes the Radiesse CaHA microspheres providing 1:1 correction and gradually dissipates leaving the microspheres at the injection site where they induce collagenesis (collagen type I and mostly collagen type III) by fibroblast activation. Animal studies have shown that this new collagen growth occurs as early as four weeks post-injection and continues for at least 12 months with an average duration of effect of 12 to 18 months, though some results have been noted 24 months post-injection. Radiesse provides both immediate (replacement volume) and long-lasting (collagen biostimulation) volume enhancement. (5) Poly-L-lactic acid PLLA is a biodegradable, bioresorbable biocompatible man-made polymer. This material has wide uses in absorbable stitches and bone screws. The effects of PLLA generally become increasingly apparent over time (over a period of several weeks) and its effects may last up to 2 years. There is an inflammatory response. PLLA is an alpha hydroxy acid polymer of the lactic acid L-enantiomeric structure that has been safely used in many applications and in medicine for more than 30 years. Its use has expanded worldwide, associated with good long-term aesthetic results thanks to its biostimulatory-collagen effect. PLLA-based fillers are supplied as a lyophilized powder to be reconstituted with sterile water. The collagen stimulatory properties were evidenced in human in subjects (n=14) who received PLLA injections (3 sessions, spaced 4 weeks apart) at the postauricular level by collagen histochemical determination on biopsies taken at different times. Increase of collagen type-I was shown at 3 and 6 months. This study opened the new class of collagen stimulators. The long duration of action was demonstrated in a first pivotal study comparing PLLA versus collagen (116/117 subjects, respectively); the long-term safety/efficacy was shown up to 25 months. The rationale for several sessions was first documented in a dedicated article; this modality allows the effect through collagen stimulation, a biological process to occur and avoids overcorrection. PLLA fillers are among the most clinically documented products. (6) Polymers, polycaprolactone The PCL-based collagen stimulator is composed of PCL microspheres suspended in a carboxymethyl-cellulose gel carrier providing immediate and sustained volumizing effects when injected; the morphology, the biocompatibility of the PCL microspheres embedded with the collagen fibers produced all contribute to the creation of a unique 3D scaffold for a sustained effect. Its safety has been investigated in clinical studies and vigilance surveys. It presents the advantage of a slower degradation than polylactic acid (PLLA) or polyglycolic acid (PGA), which both belong to the same chemical family. Both the S and M products induced collagen production. In animal, the M product induced collagen type-III and type-I at early stage (measure at 9 months), and later predominantly collagen type-I, that deposits around the PCL microspheres (measure at 21 months). Many fibroblasts were found near the PCL microspheres. Interestingly, new elastin fibers were also formed, and neovascularization with new capillaries observed as well. (7) NATURAL BIOSTIMULATORS 1. Platelet rich plasma 2. Platelet rich fibrin 3. Polynucleotides like Nucleofill or Nucleadyn 4. Exosomes 5. Alginate 6. Tropoelastin (precursor of elastin molecule) 7. Poly-y-glutamic acid Platelet-Rich Plasma (PRP): PRP treatments are produced by spinning a small volume of the patient’s own blood through a centrifuge. This separates and concentrates the blood’s components, including platelet-rich plasma and the “buffy coat,” a solution that contains immune cells. The provider combines these two components with a small amount of calcium chloride (which activates and keeps the PRP stable), then injects them into the treatment area. Over a period of months, PRP stimulates the body’s natural collagen production. Platelet-Rich Fibrin (PRF): PRF is produced using a process similar to PRP concentration. The active material is a fibrin matrix rich in platelets, stem cells, and immune cells. Like PRP, PRF treatment stimulates collagen production and is also implicated in tissue regeneration, though there’s less data on the durability of its effects. Because both treatments use material from the patient’s own body, so there’s no risk of rejection or similar complications. PRF and PRP effects are durable — typically lasting longer than 18 months. Polynucleotides: Polynucleotides are most often natural, highly purified DNA molecules extracted for example from trout gonads and activate specialised cells called myofibroblasts and adipocytes. PN containing devices act as short time temporary fillers thanks to the viscoelasticity of the long DNA fragments and improve skin well‐being (cell growth) and steady self‐repair (tissue regeneration). Read more Exosomes: The use of exosomes at the Aesthetic & Anti-Aging Medicine World Congress in Monaco was discussed during many session and some excellent results were presented. However their use is not yet approved and safety and long-term effect not yet established and largely depends on the source. Read more BOTULINUM TOXIN There is evidence that the neuromodulator or musclerelaxer Botinumtoxin after injection upregulated the expression of type I collagen, decreases the production of some MMPs in fibroblasts, preventing collagen degradation and improves collagen organisation. (8.9.) ENERGY BASED DEVICES Intense Pulsed Light/BroadBand Light, Radiofrequency Microneedling, lasers, High-Frequency Ultrasound, Electromagnetic Tec. stimulate collagen production via a controlled damage and repair mechanism. DERMO-COSMETICS WITH BIO-ACTIVES There are innovative dermo-cosmetic products containing bio-stimulating ingredients, working more superficial in comparison to in-office treatments and they therefor are potentially an excellent choice as adjunctive care for biological rejuvenation and revitalization for younger looking and acting skin. They are safe to use easy to apply over face, neck and décolletage. Unlike in-office treatments their effects are temporary (fully reversible as regulated), hence they require daily or twice daily application. Bio-stimulating active ingredients in skincare which have shown to particularly stimulate the fibroblast are for example:
VITAMIN C IS NEEDED FOR COLLAGEN SYNTHESES! Our skin needs Vitamin C to produce collagen and is not able to produce it, thus relies on external resources for supply. Therefore I highly recommend to either get enough Vitamin C from your diet or use a high quality topical product pre & post biostimulators. Read more As the biological degeneration takes place in different layers of the skin and it's underlying structures, combining in-office treatments specifically targeting those layers in a series of treatments may provide longer lasting results and give higher patient satisfaction.(13) Safety and outcome rely on the qualification and experience of your cosmetic doctor, dermatologist or plastic surgeon. Take care Special thanks MD FAAD Hassan Galadari Jair Mauricio Cerón Bohórquez M.D. References: 1. American Society Plastic Surgeons. 2020 national plastic surgery statistics; 2020. 2. Wat H, Wu DC, Goldman MP. Noninvasive body contouring: a male perspective. Dermatol Clin. 2018;36(1):49–55. 3. Wang JV, Akintilo L, Geronemus RG. Growth of cosmetic procedures in millennials: a 4.5-year clinical review. J Cosmet Dermatol. 2020;19(12):3210–3212. 4. Evaluation of the biostimulatory effects and the level of neocollagenesis of dermal fillers: a review. Haddad S, Galadari H, Patil A, Goldust M, Al Salam S, Guida S International Journal of Dermatology, 29 Apr 2022 5. J Clin Aesthet Dermatol. 2015 Jan; 8(1): 38–49. Calcium Hydroxylapatite Over a Decade of Clinical Experience Jani Van Loghem, MD, Yana Alexandrovna Yutskovskaya, MD,b and WM. Philip Werschler, MDc 6. Clin Cosmet Investig Dermatol. 2022; 15: 997–1019. Collagen Stimulators in Body Applications: A Review Focused on Poly-L-Lactic Acid (PLLA) Marie-Odile Christen Read more 7. Clin Cosmet Investig Dermatol. 2020; 13: 31–48. Polycaprolactone: How a Well-Known and Futuristic Polymer Has Become an Innovative Collagen-Stimulator in Esthetics Marie-Odile Christen and Franco Vercesi 8. Oh SH, Lee Y, Seo YJ, Lee JH, Yang JD, Chung HY, Cho BC. The potential effect of botulinum toxin type A on human dermal fibroblasts: an in vitro study. Dermatol Surg. 2012 Oct;38(10):1689-94. 9. El-Domyati M, Attia SK, El-Sawy AE, Moftah NH, Nasif GA, Medhat W, Marwan B. The use of Botulinum toxin-a injection for facial wrinkles: a histological and immunohistochemical evaluation. J Cosmet Dermatol. 2015 Jun;14(2):140-4 10 EADV 2022 Inhibition of extracellular matrix degrading enzymes and bio-stimulation of fibroblasts – A novel approach to mitigate the advanced degenerative process in skin aging Weise J, Vogelsang A, Sperling G, Welge V, Nölter A, Mielke H, Knott A, Harbig S, Stuhr A, Dunckel J, Warnke K, Geloven van A 11. EADV 2021 Multifaceted novel approach to increase skin’s own epidermal and dermal hyaluron content Bussmann T, Warnke K, Krüger A, Möller N, Harbig S, Stuhr A, Dunckel J, Geloven van A, Weise J | Beiersdorf AG, Hamburg, Germany 12. Photochemistry and Photobiology, 2005, 81: 581–587 Novel Aspects of Intrinsic and Extrinsic Aging of Human Skin: Beneficial Effects of Soy Extract Kirstin M. Su¨del et al 13. Combination Therapy in Midfacial Rejuvenation Humphrey et al. Dermatologic Surgery 42:p S83-S88, May 2016. *AMWC 2023 Tapan Patel 
It is widely known that skin´s own hyaluron is a precious molecule keeping our skin hydrated as it is a powerful humectant (attracting and binding water), hence giving the skin a natural plumpness and bounce. What many don´t know is that skin´s own hyaluronic acid content needs to be replenished continuously, as it´s half-life is only several hours up to one day 1. It´s degradation is fastened by 2 different pathways: an external influence via free radical activity or physical degradation and an internal pathway via enzymatic or biological degradation by a family of enzymes called hyaluronidase or abbreviated HYAL.
There are 6 different ones identified and HYAL 1 is the most active one. HYAL 1 “cuts” large size hyaluron molecules (the most capable of binding water) into smaller molecules, which are eliminated even faster. One of the strategies to maintain skin´s own hyaluron content is to inhibit the HYAL enzymes, especially HYAL1. Comparing photo-exposed skin to photoprotected skin showed significant increase in the expression of L-HA (low molecular weight HA) which are smaller or broken hyaluronic acid molecules. An increase of degradated hyaluron was associated with a significant expression of HYAL-1 (2)..UV, ROS or free radical activity leads to the activation of hyaluronidase (3,4). You may now wonder how it is possible that hyaluron filler injections can have a lasting effect of several months or even longer than a year. This is because in those injectable gels the hyaluron molecules are stabilized to protect them from the impact of free radicals and HYAL enzymes. Often this is done with chemical crosslinks (BDDE). Manufacturers of those hyaluron injectable gels use different stabilizing or crosslink technologies and different number of crosslinks, which impacts the gels consistency and longevity. They aren´t completely resistant to hyaluronidase, as it can be used to dissolve injected hyaluron. As hyaluron is anyway depleted and replenished every day, this dissolving procedure hardly affects skin´s own hyaluronic acid content. This is a common misconception. 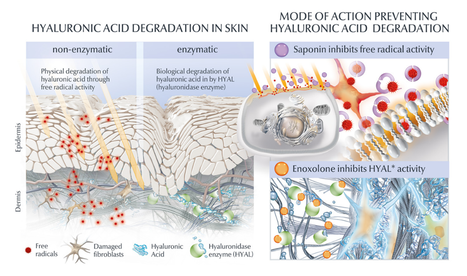
In skin care however, the use of crosslinked hyaluron (hence lasting for months or longer) does not make a lot of sense as we usually cleanse our skin twice daily and thus wash it away. It is too large to penetrate. There are some benefits for crosslinked hyaluron, but it does not impact the longevity of skin´s own hyaluronic acid content. One ingredient derived from the roots of Chinese Licorice plant called Enoxolone (also known as Glycyrrhetinic acid) however, has proven to decrease the HYAL1 activity by 54% (in vitro) (5.6). This is a novel and safe topical way to protect skin´s own hyaluronic acid content from fast degradation and elimination.
However, as mentioned before free radicals increase HYAL1 activity and as we age our skin becomes less resilient against accumulated oxidative stress. Therefore, the most optimal approach to inhibit increasing break down of hyaluronic acid is to combine HYAL1 inhibition with powerful anti-oxidants. In the illustration, which I created professionally, it is Saponin. Saponin is next to a powerful anti-oxidant, also a potent bio-stimulator of the fibroblast for hyaluron (+256%), collagen (+49%) (6) and elastin (+19%). Furthermore, Enoxolone stimulates melanin production, supports the skin's own repair mechanism against UV-induced DNA damage and inhibits enzymatic elastin degradation. What a power-couple to have in dermo-cosmetic products to manage the biological degenerative process of ageing skin. Take care 1. HA: a key molecule in skin aging E. Papakonstantinou 2. Dermatoendocrinol. 2012 Jul 1; 4(3): 253–258. doi: 10.4161/derm.21923 Hyaluronic acid: A key molecule in skin aging Eleni Papakonstantinou, 1 Michael Roth, 2 and George Karakiulakis 1 3. BMC Complementary and Alternative Medicine December 2013, 13:304| In vitro determination of the anti-aging potential of four southern African medicinal plants Authors Gugulethu NdlovuEmail, Gerda Fouche, Malefa Tselanyane, Werner Cordier, Vanessa Steenkamp 4. Bioorg Chem. 2018 Apr;77:159-167. doi: 10.1016/j.bioorg.2017.12.030. Epub 2018 Jan 4. In-vitro evaluation of antioxidant, anti-elastase, anti-collagenase, anti-hyaluronidase activities of safranal and determination of its sun protection factor in skin photoaging. Madan K1, Nanda S2. 5. EADV Poster 2021 A holistic hyaluron-centric anti-aging concept to improve static and dynamic wrinkles Geloven van A, Harbig S, Stuhr A, Dunckel J, Kuhn A, Dippe R, Warnke K, Beiersdorf AG, Hamburg, Germany 6. EADV Poster 2021 Multifaceted novel approach to increase skin’s own epidermal & dermal hyaluron content Bussmann T, Warnke K, Krüger A, Möller N, Harbig S, Stuhr A, Dunckel J, Geloven van A, Weise J, Beiersdorf AG, Hamburg, Germany 7. Hong et al. Glycyrrhetinic Acid: A Novel Modulator of Human Skin Pigmentation and DNA-Repair September 2009Journal of Investigative Dermatology Conference: 39th Annual European-Society-for-Dermatological-Research Volume: 129 
Polynucleotides (PNs) are a type of biomolecule that have recently gained traction in the field of skin care and aesthetic treatments. PNs are composed of multiple nucleotides, which are the building blocks of DNA and RNA. These biomolecules have shown promise in improving the appearance and health of the skin through their ability to stimulate cell growth (activate growth factors), tissue regeneration incl. collagen production, wound healing, fibroblast proliferation and have anti-inflammatory properties.
Polynucleotides (PN) are linear polymers composed of many nucleotide units and they play a key role in the storage and transmission of genetic information. There are two types of polynucleotides (aka nucleic acid) found in nature: ribonucleic acid (RNA) and deoxyribonucleic acid (DNA). As mentioned, PN are composed of nucleotides, which consist of 3 parts: a nitrogenous base, a phosphate group. and a five-carbon sugar (2'-deoxyribose in DNA or ribose in RNA). The five base nucleotides are adenine, guanine, cytosine, thymine, and uracil. A DNA molecule consists of two long polynucleotide chains composed of four types of nucleotide subunits: adenine, thymine, guanine, and cytosine, while RNA uses adenine, guanine, cytosine and uracil. REGENERATIVE AESTHETICS Regenerative aesthetics is an emerging branch of regenerative medicine with therapies or products aimed at recapturing youthful structure and function using the body's own systems. Examples of such treatments are platelet-rich plasma (PRP), the use of exosomes or polynucleotides. Dr. Kate Goldie explained soft tissue regeneration fundamentals as following: 1. Regeneration of tissue architecture (structure): tissue composition - component abundance, ratio's, position, density and biomechanics/integrity 2. Regeneration of tissue function: signaling, cell function, cellular components (incl. senescence), gene expression and molecular interaction. The 3 treatment pillars of regenerative aesthetics are: cells, biocues and bio-stimulatory scaffolds. Key superficial soft quiescent cells are the fibroblasts and adipose derived stem cells. One of the big advantages of regenerative aesthetics is by using the body's own system, the results are natural and focused on "skin health" (function) and "skin quality" (appearance). POLYNUCLEOTIDES IN REGENERATIVE AESTHETICS Polynucleotides are most often natural, highly purified DNA molecules extracted for example from trout gonads and activate specialised cells called myofibroblasts and adipocytes. PN containing devices act as short time temporary fillers thanks to the viscoelasticity of the long DNA fragments and improve skin well‐being (cell growth) and steady self‐repair (tissue regeneration). Studies support their dermal reactivating properties or their efficacy as “bioreactivating primers” of skin. The final outcome is more natural and in‐depth tissue regeneration and a healthier look of the skin: a more radiant complexion, even skin tone, reduced appearance of fine lines, wrinkles and sagging, faster wound healing, improved pore size and skin thickness, elasticity and hydration. Furthermore, PNs are generally well-tolerated by the skin and have a low risk of adverse effects. Their effectiveness may vary depending on the individual's skin type, age, and overall health. The long-term effects of PNs on the skin are not yet fully understood, and more research is needed to determine their safety and efficacy. There are various brands available which use polynucleotides in their (meso-) injection gels. For example Mastelli Srl, Italy NEWEST® (Polynucleotide and Hyaluronic Acid) for bio-revitalization, BR Pharm HP Cell Vitaran Skin Healers, NUCLEADYN® or Nucleofill®. One brand of (synthetic) polynucleotide-based skin care products is Yuva by Dr. Devgan Scientific Beauty. The Yuva line includes a range of products formulated with PNs, such as the Yuva Serum and the Yuva Enhancer. These products are marketed as being able to provide hydrating, anti-aging, and skin-rejuvenating benefits. THE FUTURE OF POLYNUCLEOTIDES While polynucleotides have many benefits, they also have some drawbacks. One of the primary limitations is their instability in certain environments. This instability can make it difficult to synthesize and manipulate polynucleotides in the lab. Moreover their are limitations, risks and ethical concerns harvesting or using (human identical) PN's, and long-term safety and efficacy data is not conclusive. However, PNs are a promising area of research in the field of skin care and aesthetic treatments and regeneration. We can expect to see further advancements in the development of PNs-based products and treatments. PNs are already used in combination with other biomolecules, such as hyaluronic acid, growth factors and anti-oxidants and used in combination with other treatments. For a personal recommendation on which aesthetic treatment is most suitable to aesthetically regenerate your skin, please consult an experienced board certified dermatologist, plastic surgeon or cosmetic doctor. Take care. |
CategoriesAll Acne Ageing Aquatic Wrinkles Armpits Biostimulators Blue Light & HEVIS Cleansing CoQ10 Cosmetic Intolerance Syndrome Deodorant Dermaplaning Diabetes Dry Skin Evidence Based Skin Care Exfoliation Exosomes Eyes Face Or Feet? Facial Oils Fibroblast Fingertip Units Gendered Ageism Glycation Gua Sha Hair Removal Healthy Skin Heat Shock Proteins Hormesis Humidity Hyaluron Hyaluronidase Hypo-allergenic Indulging Jade Roller Licochalcone A Luxury Skin Care Lymphatic Vessel Ageing Malar Oedema Menopause Mitochondrial Dysfunction Mood Boosting Skin Care Neurocosmetics Ox Inflammageing PH Balance Skin Photo Biomodulation Polynucleotides Psoriasis Regenerative Treatments Review Safety Scarring Sensitive Skin Skin Care Regimen Skin Flooding Skin Hydration Skin Senescence Skip-Care Sleep Slugging Sunscreen Tanning Under Eye Bags Vitamin C Well Ageing Skin Care Wound Healing Wrinkles
Archives
April 2024
|


 RSS Feed
RSS Feed
